Case Study: Management of Complications Following SCI and the Role of SLPs on a Multidisciplinary Team
Hans Schwegler, Certified Speech Therapist, Swiss Paraplegic Centre, Nottwil, Switzerland
Irene Bischof, Certified Speech Therapist, Swiss Paraplegic Centre, Nottwil, Switzerland
On a splendid, early summer’s day in June 2016, Mr. Walter had the urge to get on his mountain bike after having dinner with his wife and four school-age children. Like every evening, Mr. Walter promised to tell a bedtime story to the two younger children when he returned. So, they waited excitedly for the made-up adventures of the heroes, which Mr. Walter created from his imagination.
Mr. Walter was an avid biker and, despite being almost 50 years old, he was in exceptionally good physical condition. He loved being physically active on weekends or after a stressful day at work, breathing fresh air on forest trails, disconnecting for a while, and recharging his batteries through bike riding. Biking was his passion.
Life Changes in an Instant
WAS – because today he can only climb on his mountain bike in his thoughts, and he can only dream of challenging inclines and rapid descents. That summer day put a sudden end to his chosen sport. He had just finished his favorite bike track and was on his way home. He barely managed to avoid the cat that suddenly crossed his path. In fractions of a second, he collided with the curb and sustained a violent fall, going head first into the hard ground – completely changing his life and that of his family.
He realized immediately that something damaging had happened. For a few seconds, he was still halfway aware of the people who rushed to his help, but then it all went black. This was followed by an approximately two-week gap in his memory. At the scene of the accident, Mr. Walter required resuscitation and intubation. Initially, he was artificially ventilated [CPR] by the bystanders and the emergency physicians who fortunately arrived quickly. In the acute care clinic, where he was admitted as an emergency patient, the diagnosis showed a spinal cord injury (SCI) with complete tetraplegia (quadriplegia) sub C1 (ASIA A – complete) and, consequently, a complete failure of the respiratory muscles.
A few days after the accident, while he was still intubated and analgosedated (administration of an analgesic along with sedation), he was transported to the Swiss Paraplegic Centre (Schweizer Paraplegiker- Zentrum, hereinafter abbreviated as SPC Nottwil) for further intensive-care treatment and subsequent rehabilitation.
In light of the diagnosis and severity of the cervical spine injury, Mr. Walter was surgically tracheotomized on the second day at SPC Nottwil to prevent negative effects resulting from excessive intubation, to initiate the recovery process, and to push him towards being more actively involved in rehabilitation (Barker, J., Martino, R., Reichardt, B., Hickey, E.J., & Ralph-Edwards, A. 2009; Brown, C.V., Hejl, K., Mandaville, A.D., Chaney, P.E., Stevenson, G., & Smith, C. 2011; Durbin, 2010; Durbin, C.G., Jr., Perkins, M.P., & Moores, L.K. 2010; Flaatten, H., Gjerde, S., Heimdal, J. H., & Aardal, S. 2006; Michels, G., Motzko, M., Weinert, M., Bruckner, M., Pfister, R., & Guntinas-Lichius, O. 2014; Scheel, R., Pisegna, J.M., McNally, E., Noordzij, J.P., & Langmore, S.E. 2015; Skoretz, S.A., Flowers, H.L., & Martino, R. 2010; Skoretz, S.A., Yau, T.M., Ivanov, J., Granton, J.T., & Martino, R. 2014). The following days were marked by the reduction of the analgosedation, his slow awakening, and gradual return from his dark memory gap.
The high level of complete tetraplegia suggested that Mr. Walter would remain permanently dependent on artificial respiration.
Role of Speech Therapists
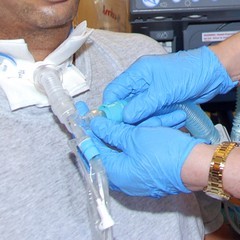
One of our tasks as speech therapists at SPC Nottwil is to help the ventilated patients regain their verbal communication skills as quickly as possible. We were, therefore, involved early-on in the intensive care unit to begin the work with the Passy Muir® Tracheostomy & Ventilator Swallowing and Speaking Valve (PMV® 007). As we worked with this patient, we provided education to explain in detail why his work with the Passy Muir® Valve (PMV®) is necessary with regard to verbal communication, as well as for the upcoming swallow-function rehabilitation. We also discussed other considerations related to tracheal suctioning, the initial air flow through the upper airway, and the possibility of insufficient exhalation, which can occur if the tracheostomy tube is too large or if there is existing stenosis. This education was provided to prepare the patient for the planned interventions and to diminish possible negative reactions he may have to change.
Even with patients who are not able to follow these explanations cognitively, we attempt treatment with the PMV 007 under strict monitoring. Often this may trigger swallowing movements and phonation. We can observe if there are any reflex reactions such as hawking or coughing, often seen secondary to secretions. Providing stimulation to the upper trachea, larynx, and pharynx with the exhaled airstream is extremely important to maintain sensitivity and awareness. Patients need this sensitivity, especially regarding swallowing. If it is absent due to an underlying neurological disease or due to a tracheostomy tube that has been cuffed too long, the risk of silent aspiration is higher, which in turn prolongs swallowing rehabilitation (Burkhead, 2011; Heidler, 2007, 2011; Heidler, Bidu, Friedrich, & Völler, 2011; Prigent et al., 2012).
On the fourth day after the tracheostomy, Mr. Walter’s respiratory situation was stable and the PEEP (positive end-expiratory pressure) on the ventilator was reduced so that the PMV 007 could be used for the first time for speech therapy. Typically, PEEP is at 8 cmH2O or lower before Valve use with this patient population. The session began with informing the patient about the planned procedure. First, oral suctioning was performed, then the cuff was deflated on the tracheostomy tube with simultaneous tracheal suctioning. It was evident that air could be exhaled through the upper respiratory tract. With the inserted PMV 007, his first attempts at articulation were still hesitant. The Philadelphia Collar (neck brace used with SCI), lingering sedatives, and some loss of air at the tracheostoma site around the tracheostomy tube, made speaking difficult for him, and his voice remained aphonic (without voice) in this first attempt.
Initially, Mr. Walter had a nasogastric tube which was replaced with a PEG tube after a few days in the ICU. The speech therapists also were instrumental in evaluating and managing Mr. Walter’s swallowing status. It had been observed that Mr. Walter had severe dysphagia as determined during the clinical diagnostic assessment. During the clinical, Mr. Walter could not swallow his own saliva. Due to the severity of his swallowing impairment, it was expected that Mr. Walter would have a prolonged swallow function rehabilitation secondary to his injury.
Because Mr. Walter began to exhibit a stable respiratory condition, he was transferred to the rehabilitation department approximately one week after entering SPC Nottwil. The daily logopedic (speech therapy) exercises focused on functional dysphagia therapy with the PMV 007 on the ventilator. These interventions for swallowing were continued after his transfer to the rehabilitation department.
Importance of Verbal Communication
With the support of the respiratory care team, including specialized nurses, two ventilation profiles with different pre-set parameters were programmed into the ventilator. The patient’s ventilator allowed for adjustments to be pre-set in profiles for specific uses by the family and staff. The first profile included the parameters for no valve use and cuff inflated. In the second profile, the parameters allowed use of the PMV 007 and the deflated cuff, which were more comfortable for the patient. By simply switching from profile one to the second profile, which allowed for PMV 007 use, the nurses and therapists could help Mr. Walter speak. After a few days, Mr. Walter shared a brief statement about his experiences while he was unable to speak. He shared:
“I have never been misunderstood as much as during the days when I could not speak. Since I can speak again, I can express my needs much better to the nursing staff. This is much better for both sides. My ability to speak is also very important for the loved ones who come to visit me. Before that, I just had to lie there like a mute fish. Now I can tell them what I think and how I feel. This is very important for them and for me.”
These statements clearly show the importance of verbal communication in an extreme situation, like the one experienced by Mr. Walter. A review of the research literature also suggests that patients with an inability to speak find it extremely stressful and frustrating (Egbers, Bultsma, Middelkamp, & Boerma, 2014; Ford & Martin-Harris, 2016; Freeman-Sanderson, Togher, Elkins, & Phipps, 2016a, 2016b; Massery, Hagins, Stafford, Moerchen, & Hodges, 2013; Sutt, Anstey, Caruana, Cornwell, & Fraser, 2017; Sutt, Cornwell, Mullany, Kinneally, & Fraser, 2015; Sutt & Fraser, 2015). The research findings support that when given the opportunity to speak, patients participate more actively in rehabilitation and feel better mentally, which results in faster progress. This ultimately illustrates how liberating it can be for those affected and how important the earliest possible implementation of a speaking valve is, even during respiratory service.
Addressing Dysphagia
In the first Fiberoptic Endoscopic Evaluation of Swallowing (FEES) study at one month post-injury, Mr. Walter’s suspected aspiration of saliva was confirmed. Therefore, the time he could stay on the PMV 007 was limited. His poor secretion management was so severe that the team felt it would be detrimental to his medical state to have his cuff deflated all day. Because of the severity, in the beginning, the PMV 007 was used only in therapy and, beginning a few days later, also with the nurses.
The gradual advances in functional dysphagia therapy resulted in more efficient saliva swallowing in the next few weeks, allowing PMV 007 use and thereby communicative capabilities to be expanded. Most of the therapy was based on the Funktionelle Dysphagietherapie (FDT) (Bartolome & Schröter-Morasch, 2018). Therapy included strength training exercises like the Masako maneuver or Mendelsohn maneuver, while swallowing training also included manipulation of the consistency of food and the use of compensatory procedures (strategies).
While practicing swallowing with small amounts of boluses, small signs of aspiration could initially be seen during tracheal suctioning. Consequently, a cautious and slow approach to dysphagia therapy was indicated. However, Mr. Walter was very motivated to practice swallowing intensively to reach one of his goals of eating again. The cleaning techniques during the swallow function training had to be continuously supported, as the severe paraplegia also caused failure of the expiratory muscles. Without support, coughing was virtually impossible, reaching a value of less than 50 L/min measured by the peak flow meter (Bach & Saporito, 1996; Torres-Castro, et al., 2014).
The loss of air next to the tracheostomy tube through the surgically created tracheostoma, unfortunately, affected his speech abilities. Several strategies were tried to improve speech, including careful positioning of the head, tracheostomy tube and breathing tube position, and slight manual pressure against the tracheostomy tube shield to reduce air loss. As is often the case, Mr. Walter’s problem of air loss through the tracheostoma also was not improved by tightening the trach ties of tracheostomy tube around the neck. This method did not improve the tracheostoma seal, but instead caused the tracheostomy tube to be pulled upwards more vigorously, increasing air leakage below the tube through the stoma. Prolonged upward movement of the tracheostomy tube also increases the risk of the tracheostoma enlarging and consequently increasing the problem of air loss. We initially hoped for a spontaneous reduction of the tracheostoma size.
Phrenic Nerve Stimulation as a Therapy
Due to the foreseeable permanent ventilation requirement, the possibility of using a phrenic nerve stimulator (Ducko, 2011) was discussed with the patient and his family in September. Initial investigations showed that the diaphragm could be stimulated bilaterally via the phrenic nerve. A purpose of the phrenic nerve stimulator is to allow ventilation to be maintained temporarily or permanently via a small pulse generator, eliminating the need to be permanently dependent on a relatively large ventilation unit that must be managed and transported around the facility all the time. Simpler handling of ventilation, through use of the stimulator, would provide Mr. Walter the prospect of more freedom of movement in everyday life.
After extensive discussions with Mr. Walter and his wife, he opted for this type of ventilation as an additional option. The surgery to implant the phrenic nerve stimulator was performed in November, almost exactly five months after his accident. About two weeks after the surgery, the phrenic nerve stimulation was initiated by the respiratory care team, and the stimulation time was gradually accelerated.
Of course, a careful and empathetic approach was necessary. Mr. Walter first had to gain the confidence that his ability to breathe could also function effectively with the stimulator. Through a long and carefully managed process, the appropriate settings had to be determined by the medical team, including the respiratory care team as a primary contributor. Throughout this process, the ventilation times on the stimulator were gradually extended. Eventually, towards the end of his rehabilitation (one year after the accident), Mr. Walter was primarily ventilated with the stimulator during the day.
Troubleshooting Changes in Swallowing and Respiration
To accelerate Mr. Walter’s use of the ventilator with the stimulator took much more time than initially considered. Ultimately, the extended time was due to circumstances that were initially undetermined by the entire care team. Shortly before the diaphragm stimulator surgery, it was observed that when eating on the ventilator, food penetration into the nasopharynx with food leakage through the nose, was observed when using the PMV 007 in-line. As the oral diet was progressed to soft consistencies, increasingly larger food items were frequently blown out through the nose, even when the settings on the ventilator were not changed. Up to this point, such problems had not occurred.
Coordination of breathing and swallowing is known to be different when eating on the ventilator (as well as under conditions on the stimulator, as will be discussed momentarily) compared to spontaneous breathing conditions. In spontaneous breathing, the person freely chooses the time of swallowing and swallow apnea (period without breath). In the controlled ventilation form, as was necessary for Mr. Walter, the breathing rhythm was predetermined by the machine. Thus, he had to add his swallowing at a suitable time in the ventilation cycle, preferably after the end of the inspiration phase, so that the subsequent exhalation helped to keep possible food residues (which had been endoscopically confirmed) away from the respiratory tract as much as possible. This coordination of breathing and swallowing required some concentration during eating, but Mr. Walter eventually mastered it.
In addition to the nasal penetrations mentioned above, the first and more frequent occurrences of difficulty during this same period were those in which exhalation was suddenly blocked while using the PMV 007, which increased stress levels. This phenomenon was inexplicable. Initially, it was found that a way to unblock the upper airway was to use active, manual, forward displacement of the lower jaw. Eventually, a rolled-up cloth positioned under the neck in a lying position proved to be an effective measure to eliminate the respiratory blockages.
In the search for causes of the nasal penetration and expiratory blockage, the available studies from radiology were evaluated. These images were made while Mr. Walter was in rehabilitation. Review of the radiology images finally identified the issue. They revealed an increasing displacement of the cervical spine. This increased the velopharyngeal distance and led to a narrowing of the exhalatory path at the base of the tongue. The narrowed conditions at the tongue base area caused the sudden respiratory blockages during exhalation while using the PMV 007. Due to the increased distance to the upper portion of the posterior wall of the pharynx, another complication had developed in that the velum could no longer fulfill its task of preventing food from entering the nose when swallowing. Eating was becoming increasingly unpleasant, tedious, and burdensome for Mr. Walter.
These circumstances accelerated the decision to undergo surgery to stiffen and stabilize the cervical spine that was urgently needed for head control during mobilized wheelchair times. Prior to these negative circumstances with eating and breathing, Mr. Walter had not been able finalize his decision about surgery. Since it was believed that the surgery to correct the position of the cervical vertebrae also may eliminate the penetration of food into the nasopharynx and the expiratory blockage, Mr. Walter finally agreed to have this surgery performed. In May 2017, 11 months after the accident, a dorsal C0-C5 spinal fusion (Spondylodesis) was performed. The time that elapsed before these issues were finally addressed also illustrates the complexity of the interlinked relationships between respiration, swallowing, and physiologic function of the upper airways. The potential significant impact had not known before the team provided comprehensive assessment of multiple areas.
After the surgery, the desired outcome was achieved. The nasal penetration disappeared, as did the exhalation blockage. Mobilization in the wheelchair was made much easier with the stabilized head posture.
Since the implementation and extension of ventilation times on the diaphragm stimulator were successful, speech therapists also had to evaluate whether swallowing while using the stimulator was sufficiently safe to do so during meals. While using the PMV 007, the ventilator creates an airflow through the larynx from the bottom to the top during the inspiratory and expiratory phases. Although this continuous airflow does not completely prevent penetration and aspiration, it does potentially counteract them. They would have to flow against the continuous airflow through the larynx into the deep respiratory tract.
When eating with the diaphragm stimulator in place, this continuous airflow from the bottom up through the larynx is non-existent. Inspiration is no longer associated with positive pressure as on the ventilator, but with negative pressure as in spontaneous breathing. If the Valve is used, most of the inspiration will flow into the lungs via the tracheostomy tube. If the tracheostomy tube is closed, inspiration flows physiologically over the larynx from top to bottom. If there is a problem with residual food while eating or residual salivation, this change to the physiological airflow increases the risk of aspiration into the deep respiratory tract.
Because of this potential problem with residual food particles, the Valve was used for Mr. Walter during initial attempts to eat with the stimulator. Even though the tracheostomy tube was closed increasingly during stimulator times, this was only done between meals. Mr. Walter shared that he enjoyed the occlusion of the tracheostomy tube because it enabled him to better smell the various odors around him. He shared that having the ability to smell odors in the environment provided some reminders of what he had previously perceived during his bike tours [rides].
One of the aspects monitored during his use of the PMV 007 trials was his blood gas. During these times, blood gas analysis showed no increase in CO2 for Mr. Walter.
Resolving the Stoma Issue
Unfortunately, the problem with the loss of air via the surgically created tracheostoma did not resolve itself, as no shrinking of the stoma occurred. Consequently, speech remained difficult for a long time and depended on the patient’s posture and positioning of the tracheostomy tube. Several alternative tracheostomy tube models had been trialed during his course of rehabilitation but did not provide a satisfactory solution. At times, various medical staff, including nursing, had to be present for Mr. Walter’s daily telephone conversations with his family to ensure sufficient voice volume while sealing the leak. Not only was this exhausting; it also affected the privacy of the patient negatively.
Therefore, a tracheostoma epithesis (functional prosthesis) was created in collaboration with an epithesis company. We were careful to use as little material as possible in the stoma around the tracheostomy tube to prevent further dilatation. Although this did not result in a perfect seal, his speech ultimately functioned with significantly less air leakage, resulting in stronger and louder voiced speech.
Progress at One Year
At the end of the one-year rehabilitation period, Mr. Walter was able to eat normal food, no longer needing any artificial nutrition or tube feeds. He continued to use his Valve during meals to provide for the best swallow function whether on the ventilator or the stimulator. The Valve was used during meals because occlusion of the tracheostomy tube has been shown to decrease residue in the pharynx during meals. Since liquids still proved to be an aspiration hazard, some of the fluids were administered via his PEG tube. With optimal posture, small boluses, and concentrated drinking, he also was able to consume some of his liquids orally.
Current Status
In August 2017, Mr. Walter moved to a nursing home near his residence. This was preceded by the respiratory care team providing intensive training to the nurses on-site. The team also provides ongoing support to the nursing home staff for questions or problems regarding respiratory ventilation. During a short, repeat rehabilitation at SPC Nottwil in early 2018, Mr. Walter underwent another FEES study to evaluate his swallowing. Unfortunately, the findings were not significantly improved, and the continued use of the Valve with meals was recommended. Caution was still required for drinking. The PEG tube is therefore still in situ. In a conversation with Mr. Walter, he shared that his two younger children now enjoy his fantasy stories again, just as much as he enjoys them himself.
This article is from the Fall 2018 International Issue of Aerodigestive Health. Click here to view Case Study: Management of Complications Following SCI and the Role of SLPs on a Multidisciplinary Team.
References
Bach, J.R., & Saporito, L.R. (1996). Criteria for extubation and tracheostomy tube removal for patients with ventilatory failure. A different approach to weaning. Chest, 110(6), 1566-1571.
Barker, J., Martino, R., Reichardt, B., Hickey, E.J., & Ralph-Edwards, A. (2009). Incidence and impact of dysphagia in patients receiving prolonged endotracheal intubation after cardiac surgery. Canadian Journal of Surgery, 52(2), 119-124.
Bartolome, G. & Schröter-Morasch, H. (2018). Dysphagia: Interdisciplinary diagnostics and rehabilitation – With access to the medical world. Frankfurt, Germany: Elsevier.
Brown, C.V., Hejl, K., Mandaville, A.D., Chaney, P.E., Stevenson, G., & Smith, C. (2011). Swallowing dysfunction after mechanical ventilation in trauma patients.
Journal of Critical Care, 26(1), 108 e109-113.
Burkhead, L.M. (2011). Swallowing evaluation and ventilator dependency – considerations and contemporary approaches. SIG 13 Perspectives on Swallowing and Swallowing Disorders (Dysphagia), 20(1), 18-22.
Ducko, C.T. (2011). Clinical advances in diaphragm pacing. Innovations (Philadelphia), 6(5), 289-297. doi: 10.1097/IMI.0b013e318237cc97
Durbin, C. G., Jr. (2010). Tracheostomy: Why, when, and how? Respiratory Care, 55(8), 1056-1068.
Durbin, C.G., Jr., Perkins, M.P., & Moores, L.K. (2010). Should tracheostomy be performed as early as 72 hours in patients requiring prolonged mechanical ventilation? Respiratory Care, 55(1), 76-87.
Egbers, P. H., Bultsma, R., Middelkamp, H., & Boerma, E. C. (2014). Enabling speech in ICU patients during mechanical ventilation. Intensive Care Medicine, 40(7), 1057-1058.
Flaatten, H., Gjerde, S., Heimdal, J. H., & Aardal, S. (2006). The effect of tracheostomy on outcome in intensive care unit patients. Acta Anaesthesiology of Scandanavia, 50(1), 92-98.
Ford, D.W., & Martin-Harris, B. (2016). I miss the sound of your voice: Earlier speech in tracheostomy patients. Critical Care Medicine, 44(6), 1234-1235. doi: 10.1097/ccm.0000000000001749
Freeman-Sanderson, A.L., Togher, L., Elkins, M. R., & Phipps, P. R. (2016a). Quality of life improves with return of voice in tracheostomy patients in intensive care: An observational study. Journal of Critical Care, 33, 186-191.
Freeman-Sanderson, A.L., Togher, L., Elkins, M.R., & Phipps, P. R. (2016b). Return of Voice for Ventilated Tracheostomy Patients in ICU: A randomized controlled trial of early-targeted intervention. Critical Care Medicine, 44(6), 1075-1081. doi: 10.1097/ccm.0000000000001610
Heidler, M.D. (2007). Rehabilitation schwerer pharyngo-laryngo-trachealer Sensibilitätsstörungen bei neurologischen Patienten mit geblockter Trachealkanüle. (Rehabilitation of severe pharyngolaryngeal tracheal sensory disturbances in neurological patients with blocked tracheostomy tube.) Neurologie & Rehabilitation,
13(1), 3-14.
Heidler, M.D. (2011). Dekanulierungs management in der Frührehabilitation (Decannulation management in early rehabilitation). Forum Logopädie, 25(3), 22-25.
Heidler, M. D., Bidu, L., Friedrich, N., & Völler, H. (2015). Oralisierung langzeitbeatmeter Patienten mit Trachealkanüle (Oralization of long-term ventilated patients with tracheostomy tube). Medizinische Klinik – Intensivmedizin und Notfallmedizin, 110(1), 55-60.
Massery, M., Hagins, M., Stafford, R., Moerchen, V., & Hodges, P. W. (2013). Effect of airway control by glottal structures on postural stability. Journal of Applied Physiology (1985), 115(4), 483-490.
Michels, G., Motzko, M., Weinert, M., Bruckner, M., Pfister, R., & Guntinas-Lichius, O. (2014). Management of dysphagia in internal intensive-care medicine. Med Klin Intensivmed Notfmed. doi: 10.1007/s00063-014-0386-8
Prigent, H., Lejaille, M., Terzi, N., Annane, D., Figere, M., Orlikowski, D., & Lofaso, F. (2012). Effect of a tracheostomy speaking valve on breathing-swallowing interaction. Intensive Care Medicine, 38(1), 85-90.
Scheel, R., Pisegna, J.M., McNally, E., Noordzij, J.P., & Langmore, S.E. (2015). Endoscopic assessment of swallowing after prolonged intubation in the ICU setting. Annals of Otology, Rhinology, and Laryngology. 125(1), 43-52.doi: 10.1177/0003489415596755.
Skoretz, S.A., Flowers, H.L., & Martino, R. (2010). The incidence of dysphagia following endotracheal intubation: A systematic review. Chest, 137(3), 665-673.
Skoretz, S.A., Yau, T.M., Ivanov, J., Granton, J.T., & Martino, R. (2014). Dysphagia and associated risk factors following extubation in cardiovascular surgical patients. Dysphagia, 29(6), 647- 654.
Sutt, A.L., Anstey, C.M., Caruana, L.R., Cornwell, P.L., & Fraser, J.F. (2017). Ventilation distribution and lung recruitment with speaking valve use in
tracheostomised patient weaning from mechanical ventilation in intensive care. Journal of Critical Care, 40, 164-170.
Sutt, A.L., Cornwell, P., Mullany, D., Kinneally, T., & Fraser, J F. (2015). The use of tracheostomy speaking valves in mechanically ventilated patients results in improved communication and does not prolong ventilation time in cardiothoracic intensive care unit patients. Critical Care, 30(3), 491-4. doi: 10.1016/j.jcrc.2014.12.017.
Sutt, A.L., & Fraser, J.F. (2015). Speaking valves as part of standard care with tracheostomized mechanically ventilated patients in intensive care unit. Critical Care, 30(5), 1119- 1120.
Torres-Castro, R., Vilaro, J., Vera-Uribe, R., Monge, G., Aviles, P., & Suranyi, C. (2014). Use of air stacking and abdominal compression for cough assistance in people with complete tetraplegia. Spinal Cord, 52(5), 354-357.












